Author: Mr Chad Chang FRCS(Plast), Consultant Plastic Surgeon
Review Status: Peer-reviewed by Mr John Henton FRCS(Plast), Consultant Plastic Surgeon
Published: 10 March 2026
Quick Summary: Standard lymphoedema assessments rely on tape measures, which track limb volume but cannot identify the physiological cause of the swelling. Indocyanine Green (ICG) lymphography is a dynamic, radiation-free imaging technique that visualises lymphatic flow in real-time. This guide explains the procedure, the specific patterns identified during a scan, and why expert interpretation is vital for safe surgical planning.
Why is visualisation better than a tape measure?
Living with unexplained swelling or facing a lymphoedema diagnosis often brings uncertainty. If you have attended a standard clinic, your assessment likely involved a tape measure, a physical examination, and a history review.
While these tools are necessary, they have a key limitation: they confirm the limb is swollen, but they cannot show why or where the drainage problem lies. For patients with complex swelling or those considering surgical treatment, relying solely on a “blind” surface assessment is insufficient. Modern management requires visualising the lymphatic system beneath the skin to provide definitive answers.
What Is ICG Lymphography?
ICG lymphography is a diagnostic imaging technique that allows clinicians to see superficial lymphatic vessels functioning in real-time. It differs significantly from other historical scanning methods:
- Lymphoscintigraphy: Uses radioactive tracers to create static, often blurry images of the lymph nodes.
- MR Lymphography/Lymphangiography: Provides a detailed structural snapshot of tissues but lacks dynamic, real-time flow data.
- ICG Lymphography: A dynamic test showing the flow and function of the system as it happens.
How the procedure works
- The Dye: A tiny amount of Indocyanine Green (a medical dye) is injected just under the skin. This dye binds to proteins in the lymph fluid and travels specifically through the lymphatic vessels.
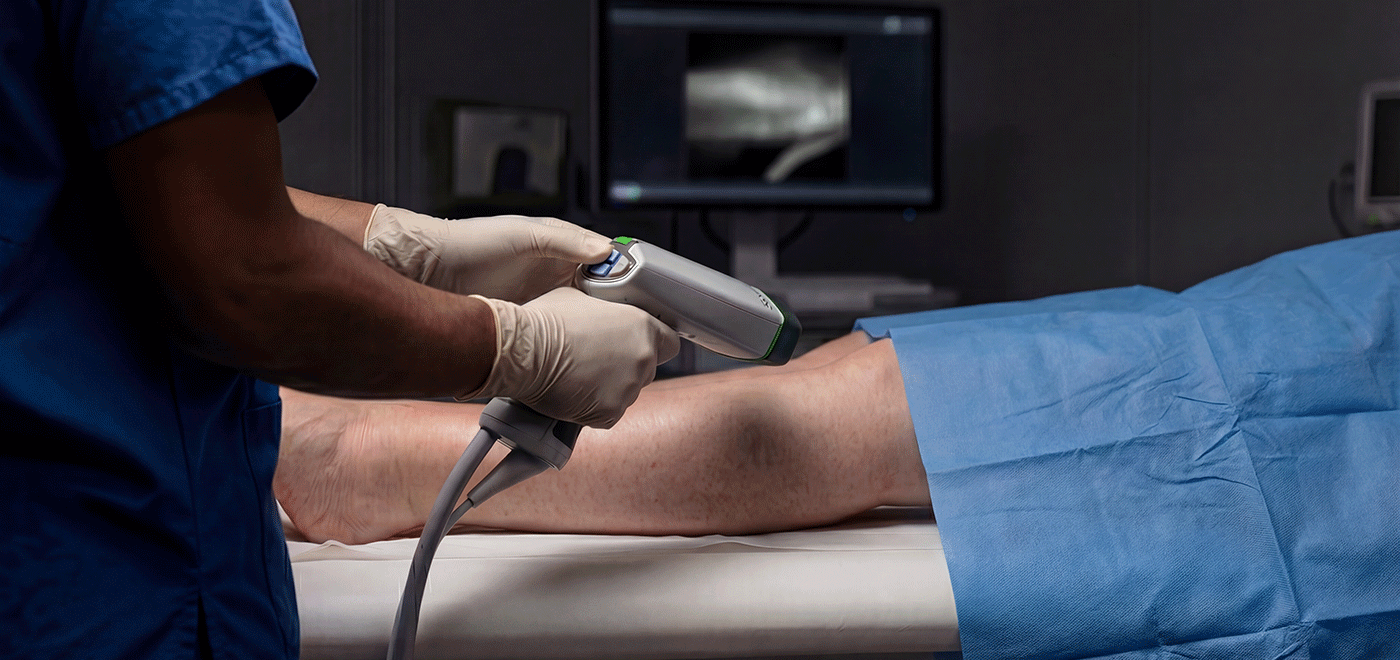
- The Camera: We use a specialised near-infrared camera system. To the naked eye, nothing changes on the skin surface, but on the screen, the dye fluoresces brightly.
- The Map: We observe the dye travelling up the limb. This allows us to identify individual pumping vessels, measure the speed of transport, and pinpoint the exact locations where flow stops, leaks, or fails.
What do the ICG scan patterns mean?
A common misconception is that the camera machine itself provides the diagnosis. In reality, ICG lymphography is highly operator-dependent; it requires an experienced specialist to interpret the movement of the dye.
| ICG Pattern | Visual Appearance | Clinical Significance |
|---|---|---|
| Linear Flow | Straight, well-defined lines moving quickly up the limb. | Healthy System: Confirms intact superficial lymphatics; helps rule out primary failure. |
| “Splash” or “Stardust” | Fine leakage out of the vessels into the surrounding skin. | Leakage: Indicates vessels are under pressure but still functional. Ideal for LVA planning. |
| Diffuse Spread | Dye spreads out like a cloud (dermal backflow). | Pump Failure: Fluid is pushed back into the skin. Prevents “blind” surgical attempts. |
Who Needs This Scan?
Not every patient with mild swelling requires advanced mapping. However, in a specialist practice, it is essential for three specific groups:
1. The "Unclear Diagnosis"
Some swelling profiles do not fit standard rules, such as lipo-lymphoedema (a fat disorder presenting with fluid symptoms) or subtle post-cancer swelling with borderline measurements. ICG provides objective confirmation of lymphatic failure through backflow patterns, or definitively rules it out if the flow is healthy.
2. The Surgical Candidate
If you are considering any form of surgery for lymphoedema or lipoedema, operating blindly introduces unnecessary risk. The scan helps us decide which surgery is appropriate:
- For LVA: If the scan reveals functioning vessels that are struggling (leaking or blocked), you may be a candidate for Lymphaticovenous Anastomosis (LVA). Here, the scan acts as a GPS map. It allows us to mark the exact location of these working vessels on your skin so we can target them through tiny incisions and bypass the blockage.
- For VLNT: Sometimes, the scan shows significant fluid buildup (dermal backflow) but no functioning vessels suitable for LVA. In these cases, simple bypasses would not work because there is no “pipe” to connect. Vascularised Lymph Node Transfer (VLNT) can bring in healthy tissue to act as a new pump and potentially promote lymphatic regeneration.
- For Liposuction: If the scan shows that most of the lymphatic vessels are no longer functional and the limb is solid and fibrotic, the goal shifts to removing the bulk. Here, the ICG map allows us to visualise the remaining intact lymphatic drainage pathways to ensure we protect them during the procedure, preserving your remaining function.
3. The High-Risk Monitoring Group
For patients at high risk of developing secondary lymphoedema, including breast cancer-related lymphoedema (BCRL) or lower limb lymphoedema following treatment for pelvic, gynaecological, or urological cancers such as prostate cancer, optional interval ICG lymphography can be offered.
This proactive approach monitors superficial lymphatic transport closely in the arms or legs to identify early, sub-clinical changes, such as dermal backflow, before swelling becomes permanent or tissue changes occur. As this is not currently routine in standard care, we discuss the potential benefits and limitations with each person to determine if interval mapping will add useful information to their specific situation.
Is ICG Lymphography Safe?
ICG is considered very safe and has been used in medicine (for heart and liver testing) for decades.
- Radiation-Free: Unlike nuclear medicine scans, there is no radiation exposure.
- Pain: The injection uses a very fine needle. Most patients report a mild sting that lasts a few seconds.
- Allergies: The dye contains iodine. It is not suitable for patients with a known iodine allergy or those with an overactive thyroid. We screen for this carefully before every appointment.
Next Steps: Managing Your Lymphatic Health
If you have struggled to obtain a clear answer regarding the cause of your swelling, or if you are reading conflicting advice online, a specialist assessment is the appropriate next step.
- Arrange a Clinical Consultation: A specialist review includes a detailed history and physical examination to determine if advanced mapping is indicated.
- Submit Relevant Records: Provide previous clinic letters and imaging reports to ensure a focused, efficient diagnostic plan.
- Evaluate Monitoring Options: Patients who have recently completed cancer treatment may discuss interval ICG lymphography as part of a surveillance programme.
To discuss your case or arrange an assessment at the Great North Lymphatic Centre (GNLC), contact the team to review your imaging and clinical history to advise on the role of lymphoedema surgery in your care.
Disclaimer: This content is for educational purposes only and does not constitute personal medical advice. Content written by Mr Chad Chang and peer-reviewed by Mr John Henton.
